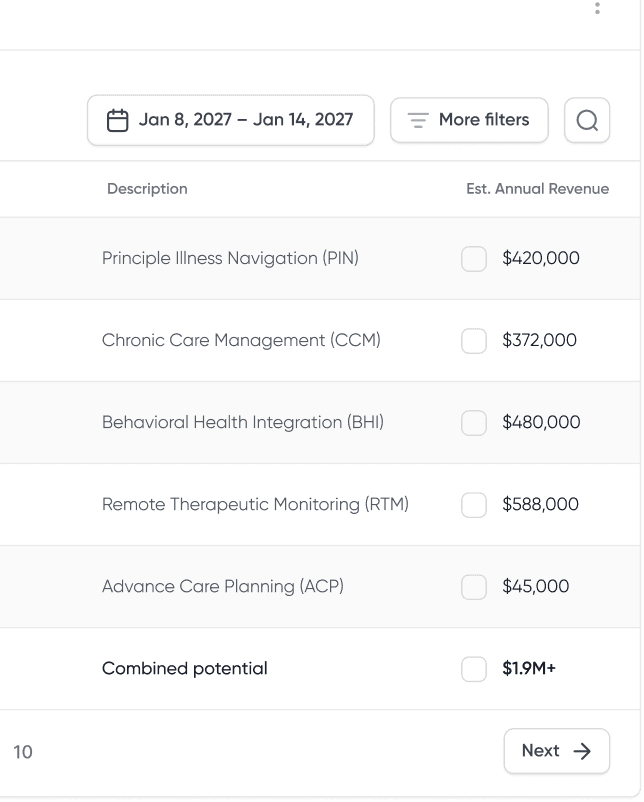
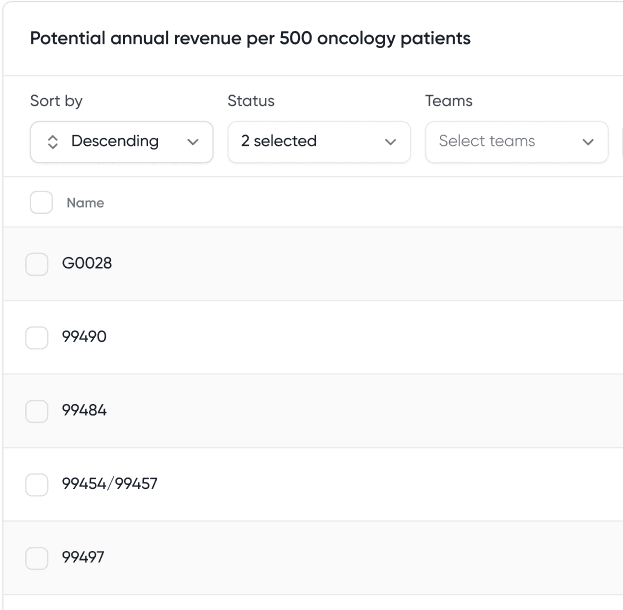
Standardize navigation at scale
Fidari unifies how navigation is delivered across every site, service line, and role. One workflow, one documentation standard, one source of truth. It works the same whether you operate a single community hospital or a multi-site cancer network.